How to Reduce Optical Billing Errors: A 10-Minute Guide for Optometry and Ophthalmology Practices
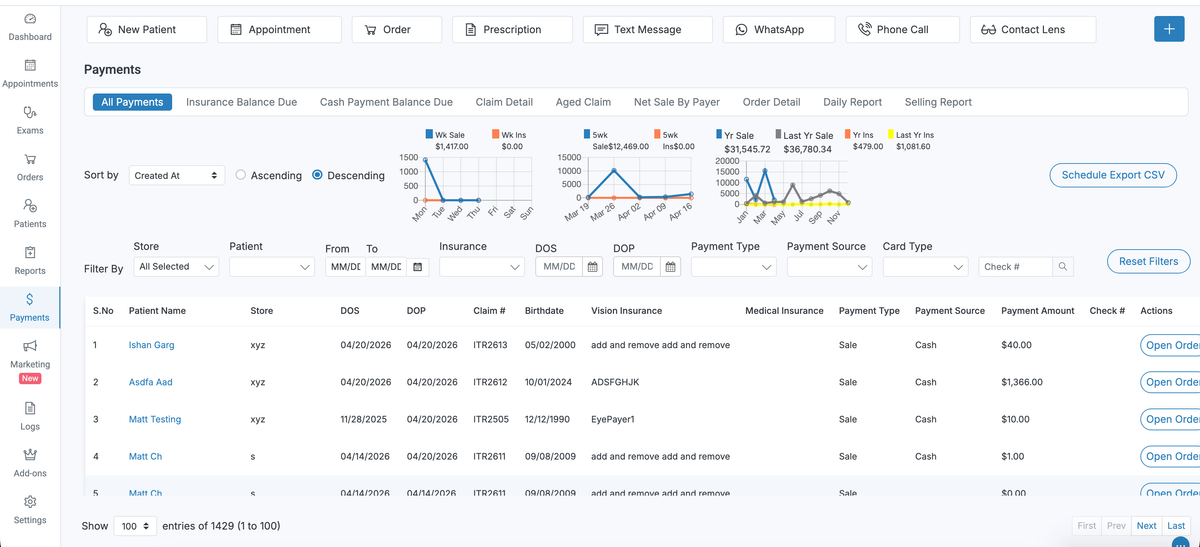
How to Reduce Optical Billing Errors: A 10-Minute Guide for Optometry and Ophthalmology Practices
Optical billing errors usually do not come from one dramatic mistake. They come from a chain of small failures: the wrong payer gets billed, coverage is classified incorrectly, documentation does not fully support medical necessity, modifiers are added too casually, or a noncovered service is never handled correctly before the claim goes out. CMS has repeatedly emphasized that many improper payments are tied to missing administrative steps or insufficient documentation, not just overt fraud or abuse, and eye care is a specialty area where documentation, coverage, coding, and supervision rules can break down quickly.
That is why the best-performing optical practices do not treat billing as a back-office cleanup job. They build billing accuracy into the entire patient journey: scheduling, eligibility verification, check-in, clinical documentation, charge capture, claim submission, denial review, and staff retraining. When you do that, errors drop because the workflow itself starts preventing bad claims before they are created.
1) Separate medical, vision, and noncovered workflows before the patient is even seen

One of the biggest sources of optical billing error is treating every eye visit as if it belongs in one billing bucket. It does not. Eye care sits at the overlap of medical services, vision benefits, and services that may be noncovered depending on payer rules. CMS’s Medicare Vision Services guidance makes clear that some vision-related services have very specific coverage conditions, while other services, including routine refraction, are not covered by Medicare in the ordinary sense. If your staff does not distinguish these categories early, the claim is already at risk before the exam starts.
Best practice is simple: build a pre-visit decision tree. Every appointment should be classified in advance as medical eye problem, routine/vision, mixed visit requiring careful payer handling, or likely noncovered service. That reduces front-desk improvisation and keeps staff from guessing after the encounter is over. It also makes patient financial conversations cleaner because the coverage path is being decided before the chart is touched.
2) Verify eligibility, coordination of benefits, and payer hierarchy before check-in
A surprising number of claims fail because the practice had the wrong payer order, outdated coverage data, inactive benefits, or an unresolved coordination-of-benefits problem. CMS billing education for professional claims explicitly ties successful claim submission to correct enrollment, claim filing, and coordination of benefits processes. In plain English: a clean claim still fails if it goes to the wrong payer or carries the wrong insurance structure.
The operational fix is to stop treating eligibility as a same-day courtesy. Verify coverage before the visit, confirm it again at check-in, and require staff to validate payer priority, subscriber details, plan type, and any vision-versus-medical carve-outs. In eye care, that matters more than in many specialties because patients often assume “eye coverage” is one thing when the billing reality is split across multiple benefit structures. A practice that verifies this 24 to 48 hours in advance will prevent a huge amount of avoidable rework.
3) Make documentation drive the claim, not memory

CMS documentation guidance is blunt on this point: claims must be supported by the medical record, and incomplete or insufficient records are a common reason claims fail review. CMS also separately reminds providers that required signatures, attestations, and record integrity matter during review. The CDC’s ICD-10-CM guidance likewise stresses that complete, consistent documentation is the foundation of accurate coding.
For optical practices, that means the coding team should never be “reconstructing” the visit from habit, assumptions, or half-finished notes. The claim should come from what is clearly documented in the chart: the reason for the visit, the findings, the assessment, the medical necessity, and the exact services actually performed. If a chart cannot support the code cleanly, the answer is not to “push it through.” The answer is to fix the documentation before billing. That one discipline alone can reduce downstream denials, refunds, rebills, and audit exposure.
4) Train diagnosis specificity like it is revenue protection, because it is
Diagnosis coding in eye care is rarely just a clerical step. It is often the bridge between the clinical story and the payer’s medical-necessity logic. CDC’s ICD-10-CM guidance makes clear that coding should reflect the specific reason for the encounter and the conditions treated, and that accurate coding depends on complete documentation. In an eye-care setting, vague or incomplete diagnoses can easily break the link between the exam, testing, and payer coverage expectations.
That is why practices should train providers and scribes to document specificity consistently: laterality when relevant, acute versus chronic status when supported, relationship between symptoms and findings, and the medical reason diagnostic testing was necessary that day. The more specific and internally consistent the diagnosis documentation is, the less likely your billers are to rely on guesswork, generic templates, or payer roulette.
5) Get serious about modifier discipline

Modifier misuse is one of the fastest ways to turn a valid clinical encounter into a billing problem. CMS’s NCCI policy framework exists specifically to reduce incorrect coding combinations and inappropriate separate billing, and CMS has published specialty-specific billing education showing that even common ophthalmic scenarios can be misbilled when E/M services and procedures are reported incorrectly. Academic compliance guidance from UTHealth and Rochester reinforces the same point: modifier -25 is not supposed to be a reflex; it must reflect a truly significant, separately identifiable E/M service beyond the work already included in the procedure.
The real best practice is to require a short internal justification rule for high-risk modifiers. If a biller or coder cannot explain in one or two sentences why the modifier is supported by the documentation, it should not be on the claim yet. That discipline alone cuts down a lot of “we always bill it this way” behavior, which is exactly the kind of pattern that creates audits and recoupments later.
6) Treat ABNs and noncovered service workflows as part of patient communication, not last-minute paperwork
When Medicare is not likely to cover an item or service, CMS requires proper notice workflows, and CMS’s ABN materials make clear that if required notices are not handled properly, the provider may end up financially liable. In eye care, this matters because practices regularly touch services with limited, conditional, or excluded coverage. The billing mistake is often not only that the claim was wrong, but that the patient communication and documentation trail were also wrong.
Strong practices handle this early and consistently. They identify likely noncovered services before the encounter is completed, deliver the proper financial notice process when required, document the decision cleanly, and make sure the billing path matches what the patient was told. That prevents two expensive problems at once: payer denials and patient disputes. It also protects trust, which matters because a technically correct claim can still feel like a billing failure if the patient never understood the coverage issue in the first place.
7) Stop cloned notes, copy-forward abuse, and sloppy template use

This is the EHR problem nobody likes talking about. HHS OIG has warned for years that EHR features can create vulnerabilities around authorship, overdocumentation, and copied language, and reported that only about a quarter of hospitals in one review had policies addressing copy-paste. OIG also found that many contractors were not well-equipped to determine whether documentation had been copied or overdocumented. In other words, cloned documentation is not just a chart-quality issue. It is a billing integrity issue.
In optical settings, cloned notes are especially dangerous because they can make every visit look medically identical, which weakens the credibility of your coding and medical-necessity story. The fix is not to ban templates. The fix is to use templates correctly: standardize structure, but require encounter-specific edits for history, assessment, testing rationale, plan, and any separately billed work. Templates should speed up compliant documentation, not mass-produce it.
8) Keep provider enrollment, revalidation, and billing privileges clean
Some claim problems have nothing to do with the visit itself. CMS states that failing to revalidate on time can place Medicare reimbursement on hold or deactivate billing privileges, and if billing privileges are deactivated, Medicare generally will not reimburse for services during the deactivated period. That is not a coding error. That is an operational own goal.
For growing optical groups, this becomes more important as locations, providers, and service lines expand. Someone in the organization should own payer enrollment hygiene as a formal revenue-cycle function, with ticklers for revalidation dates, NPI/PECOS accuracy, location changes, reassignment updates, and payer roster audits. A practice can have excellent documentation and still lose revenue if the enrollment side is messy.
9) Build a denial feedback loop that actually changes behavior

CMS’s improper-payment materials emphasize that many problems arise from missing administrative steps or insufficient information. That should change how practices look at denials. A denial is not just an account to rebill. It is a signal telling you where the workflow failed. If you only fix the individual claim, you preserve the same broken process that created it.
The better model is to review denials weekly by root cause: eligibility, authorization, diagnosis specificity, modifier logic, documentation gap, noncovered-service handling, enrollment issue, or simple data-entry failure. Then tie each category to one owner and one corrective action. Over time, your denial dashboard should become a training roadmap. That is how you move from reactive billing to a system that gets smarter every month.
10) The highest-leverage workflow change: create a pre-bill compliance checkpoint
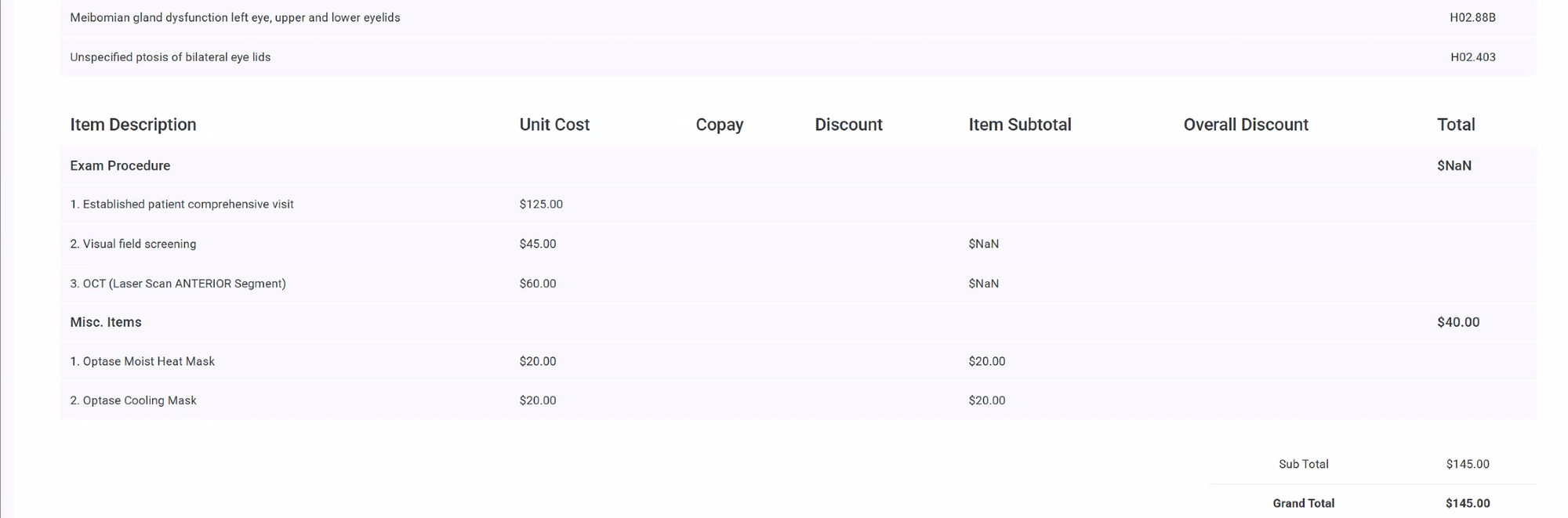
If you want the single best operational move, it is this: add a short pre-bill checkpoint for visits that are most likely to blow up later. Mixed medical/vision visits, testing-heavy encounters, procedure-plus-E/M days, likely noncovered services, and anything involving unusual modifiers should all pass through a quick standardized review before final claim release. That review does not need to be heavy. It just needs to confirm five things: correct payer path, documentation support, diagnosis specificity, modifier support, and patient financial handling.
This kind of checkpoint is where serious optical groups separate themselves. It reduces preventable denials, improves cash flow quality, lowers refund risk, and creates a cleaner record if claims are ever reviewed. More importantly, it takes billing accuracy out of the realm of heroics and turns it into process design. That is where the real gains come from.
Final takeaway
Reducing optical billing errors is not about finding a better biller to clean up bad claims after the fact. It is about engineering a better system before the claim exists. Separate the coverage path early. Verify benefits before the patient arrives. Make documentation drive coding. Enforce diagnosis specificity. Use modifiers with discipline. Handle noncovered services correctly. Control EHR note integrity. Maintain provider enrollment. Audit denials by root cause. Add a pre-bill checkpoint for high-risk encounters. Do those things consistently, and billing accuracy improves because the workflow stops producing junk.
References / Backlink URLs
- CMS Medicare Vision Services
https://www.cms.gov/outreach-and-education/medicare-learning-network-mln/mlnproducts/downloads/visionservices_factsheet_icn907165.pdf - CMS Complying With Medical Record Documentation Requirements
https://www.cms.gov/files/mln909160-complying-with-medical-record-documentation-requirements.pdf - CMS Complying With Medicare Signature Requirements
https://www.cms.gov/files/document/mln905364-complying-medicare-signature-requirements.pdf - CDC ICD-10-CM Files
https://www.cdc.gov/nchs/icd/icd-10-cm/files.html - CDC ICD-10-CM Overview
https://www.cdc.gov/nchs/icd/icd-10-cm/index.html - CDC FY 2026 ICD-10-CM Guidelines
https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Publications/ICD10CM/2026-update/ICD-10-CM%20April%201%202026%20Guidelines%20Final.pdf - CMS Medicare Billing: 837P and Form CMS-1500
https://www.cms.gov/files/document/837p-cms-1500pdf - CMS Medicare Advance Written Notices of Non-coverage
https://www.cms.gov/files/document/mln006266-medicare-advance-written-notices-non-coverage.pdf - CMS ABN Form Instructions
https://www.cms.gov/medicare/medicare-general-information/bni/downloads/abn-form-instructions.pdf - CMS Medicare Claims Processing Manual
https://www.cms.gov/regulations-and-guidance/guidance/manuals/downloads/clm104c30.pdf - CMS NCCI Policy Manual for Medicare Services
https://www.cms.gov/files/document/2025nccimedicarepolicymanualcompletepdf.pdf - CMS Evaluation and Management Services & Intravitreal Injections: Bill Correctly
https://www.cms.gov/outreach-and-education/medicare-learning-network-mln/mlnproducts/fast-facts/evaluation-management-services-intravitreal-injections-bill-correctly - CMS Revalidations (Renewing Your Enrollment)
https://www.cms.gov/medicare/enrollment-renewal/providers-suppliers/revalidations - CMS Medicare Provider Enrollment
https://www.cms.gov/Outreach-and-Education/Medicare-Learning-Network-MLN/MLNProducts/EnrollmentResources/provider-resources/provider-enrolment/Med-Prov-Enroll-MLN9658742.html - CMS Medical Record Maintenance & Access Requirements
https://www.cms.gov/files/document/mln4840534-medical-record-maintenance-and-access-requirements.pdf - CMS FY 2024 Improper Payments Fact Sheet
https://www.cms.gov/newsroom/fact-sheets/fiscal-year-2024-improper-payments-fact-sheet - HHS OIG: EHR Vulnerabilities and Program Integrity
https://oig.hhs.gov/reports/all/2014/cms-and-its-contractors-have-adopted-few-program-integrity-practices-to-address-vulnerabilities-in-ehrs/ - HHS OIG: Copy-Paste and EHR Fraud Safeguards
https://oig.hhs.gov/reports/all/2013/not-all-recommended-fraud-safeguards-have-been-implemented-in-hospital-ehr-technology/ - McGovern Medical School: Complying with Eye Care Guidelines
https://med.uth.edu/mshbc/specialty-coding-compliance/complying-with-eye-care-guidelines/ - McGovern Medical School: E/M + Procedure = Modifier -25
https://med.uth.edu/mshbc/2022/11/17/e-m-procedure-modifier-25/ - University of Rochester Medical Center: Modifier 25 – E&M on the Same Day as a Procedure
https://www.urmc.rochester.edu/MediaLibraries/URMCMedia/compliance-office/education-tools/em-guidelines/em-modifier-25.pdf